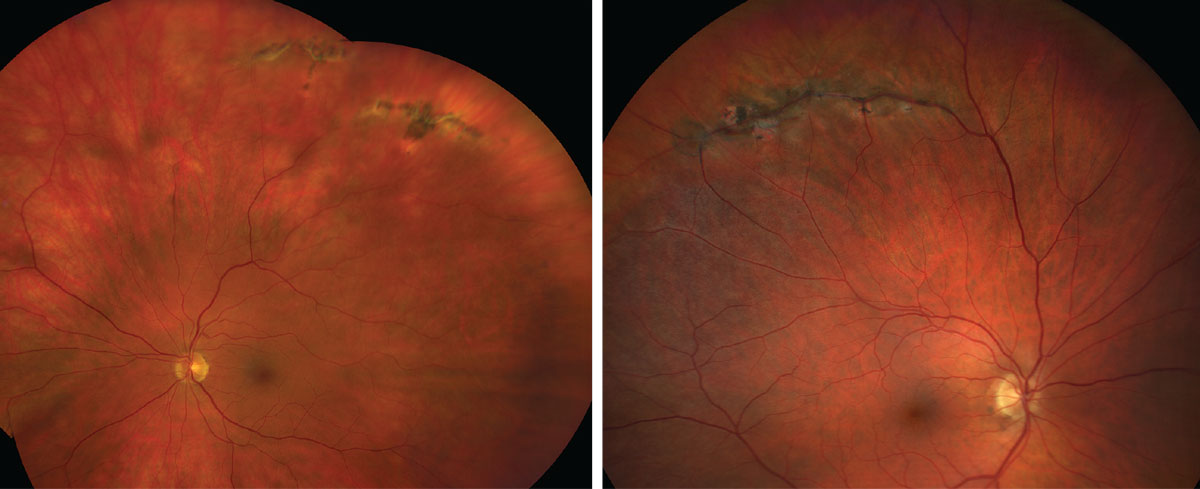
In addition, patients with lattice degeneration are at increased risk of developing atrophic retinal holes that may lead to slowly progressive RD without symptoms until more central vision is affected. Patients should be carefully examined and monitored during acute PVD events. Patients with lattice degeneration should be thoroughly educated about symptoms of acute PVD such as flashes of light and new-onset floaters. 8,9 As patients age and undergo posterior vitreous detachment (PVD), areas of lattice degeneration are prime locations for retinal breaks to occur. Lattice represents thin areas of retina, and these regions often have dense vitreous adhesions. 
Lattice degeneration can lead to trouble in multiple ways. Although the overall risk is low (around 1%), lattice degeneration and atrophic retinal holes are responsible for about 30% of RDs. Patients with lattice degeneration have increased risk for retinal detachment (RD). Technically, the most common type of peripheral retinal degeneration is microcystoid degeneration, but lattice degeneration is a more clinically significant finding that occurs in about 10% of the population. PERIPHERAL RETINAL DEGENERATION: LATTICE DEGENERATION As CHRPE develop lacunae there is RPE atrophy. OCT (bottom) shows thickening of the RPE and atrophy of the outer retina without evidence of a choroidal lesion (blue arrows demonstrate the boundaries of the lesion). CHRPE shows dense hypo-autofluorescence on FAF (B). OCT (bottom) confirms that the lesion is flat and located within the choroid. FAF (top right) shows no alteration to the FAF signal, demonstrating no presence of lipofuscin accumulation. Small, flat nevus adjacent to the optic nerve (A). 5 Although the risk of conversion to a malignant lesion is not zero, it is significantly less than for nevi, and these lesions typically do not require as frequent observation (Figure 1). OCT will show atrophy of the outer retina overlying the lesion, and they will be hypoautofluorescent on FAF. These flat lesions of the RPE will be visible with red-free or green filter. Nevi may be confused with another frequently encountered lesion: congenital hypertrophy of the retinal pigment epithelium, or CHRPE. Nevi may create mottled autofluorescence due to disruption of the overlying retinal pigment epithelium (RPE), but orange pigment composed of lipofuscin will be highly hyperautofluorescent. Fundus autofluorescence (FAF) can be used to look for the presence of orange pigment. 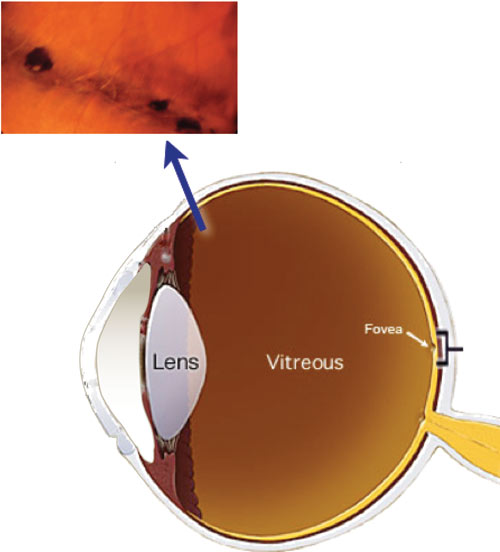
OCT can be used to document nevus size and thickness and to evaluate for overlying drusen or subretinal fluid. These signs have been turned into the catchy pneumonic: To find small ocular melanoma, use helpful hints daily. The following signs should draw concern for melanoma: thickness >2 mm, subretinal fluid, visual symptoms, orange pigment, margins ≤3 mm from the disc, ultrasonographic hollowness, absence of halo, and absence of drusen. As these are lesions in the choroid, they disappear or are much less evident with use of a red-free or green filter than with use of white light.Īlthough conversion of a nevus to choroidal melanoma is rare, patients should be monitored for signs of this occurrence. These are benign tumors composed of melanocytes, and they occur in about 3% to 10% of the population. POSTERIOR SEGMENT TUMOR: NEVUSĬhoroidal nevus is the most common intraocular tumor. In this article, I highlight some of the retina’s most common culprits. There are more off-the-wall retinal lesions documented than anyone could ever fully keep track of, but on a daily basis we are much more likely to encounter certain “usual suspects.” It is important to know how to identify these common lesions and differentiate them from other conditions. They may be tumorous, vascular, degenerative, inflammatory, traumatic, or even infectious. This knowledge can also better equip us to understand when a lesion doesn’t fit the profile of one of the usual suspects.Ī lesion is defined as “an abnormal change in structure of an organ or part due to injury or disease.” 1 Lesions in the retina can occur from numerous etiologies.Knowing the presentations of these most common lesions can help clinicians refer promptly when necessary.There are numerous retinal lesions, but some “usual suspects” are encountered frequently in the clinic.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
